The demand for accurate and compliant billing in behavioral health has never been higher. From mental health clinics to addiction treatment centers, providers face constant pressure to manage complex coding, changing regulations, and insurance challenges. Choosing a professional behavioral health billing company is no longer optional—it’s a strategic move to protect revenue and ensure operational efficiency.
Behavioral health billing is fundamentally different from general medical billing. It involves unique CPT codes, strict documentation requirements, and frequent payer scrutiny. Without expertise, even small errors can lead to claim denials, revenue leakage, or compliance risks.
This blog explores how a professional partner can transform your billing operations and why outsourcing is becoming the preferred choice across the United States.
Why Behavioral Health Billing Is More Complex Than General Medical Billing
Behavioral health billing requires specialized knowledge due to its distinct nature. Unlike standard procedures, mental health services often involve time-based coding, therapy sessions, and evolving treatment plans.
Key challenges include:
Frequent claim denials due to documentation gaps
Complex coding structures for therapy and psychiatric services
Strict payer policies for mental health claims
Prior authorization requirements
Managing patient confidentiality and compliance
This is why many providers are turning to a behavioral health billing agency that understands these nuances deeply.
What Does a Professional Behavioral Health Billing Company Do?
A professional behavioral health billing company handles the complete revenue cycle—from patient intake to final payment posting. Their goal is to reduce administrative burden while maximizing reimbursement.
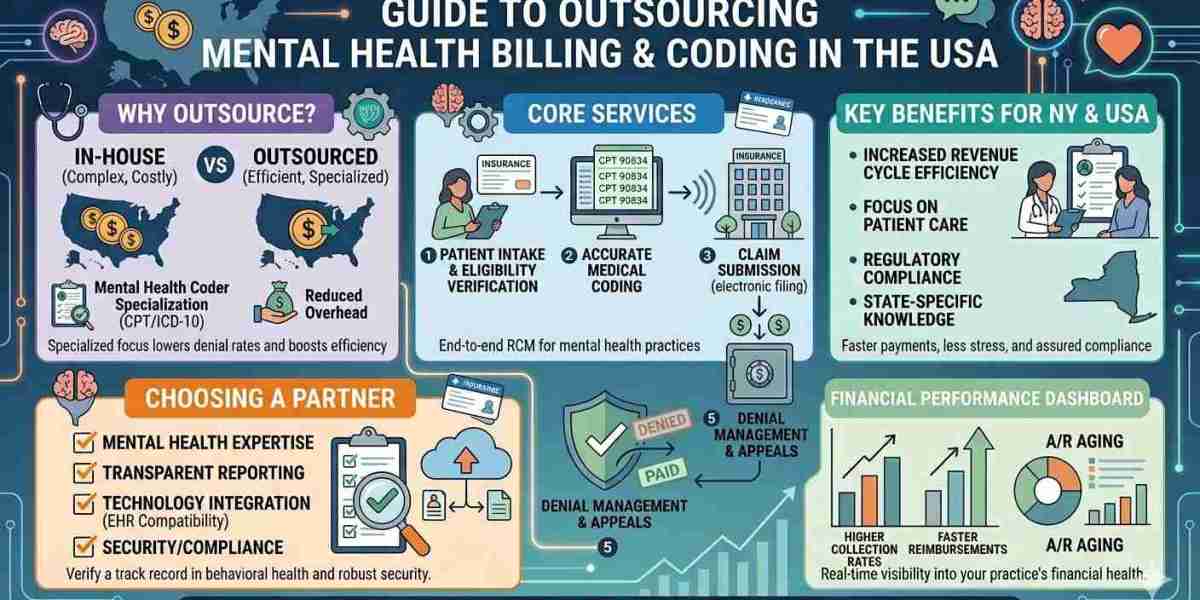
Core services include:
Insurance verification and eligibility checks
Accurate coding for behavioral health procedures
Claim submission and tracking
Denial management and appeals
Payment posting and reporting
Compliance monitoring
These services are often bundled into comprehensive behavioral health billing solutions designed to improve cash flow and operational efficiency.
Benefits of Outsourcing Behavioral Health Billing
Many healthcare providers now outsource behavioral health billing services to specialized companies instead of managing it in-house. This shift is driven by both cost and performance advantages.
Improved Revenue Cycle Performance
Outsourcing reduces claim errors and speeds up reimbursements. A top outsource behavioral health billing company ensures claims are clean before submission.
Access to Expert Coders
Professional teams stay updated with the latest CPT, ICD-10, and payer-specific guidelines, ensuring accurate medical billing behavioral health processes.
Cost Efficiency
Hiring and training in-house billing staff can be expensive. Outsourcing behavioral health billing and coding eliminates overhead costs.
Better Compliance
Regulatory requirements in mental health billing are strict. A professional partner ensures compliance with HIPAA and payer guidelines.
Focus on Patient Care
By delegating billing tasks, providers can focus more on delivering quality care rather than administrative work.
How to Choose the Best Behavioral Health Billing Services Company
Selecting the right partner is critical. Not all providers offer the same level of expertise or service quality.
Consider the following factors:
Experience in behavioral & mental health billing services
Proven track record with mental health providers
Transparent pricing structure
Advanced technology and reporting tools
Strong denial management process
Customizable behavioral health billing service options
A best behavioral health billing services company will act as a strategic partner, not just a vendor.
State-Specific Expertise Matters in Behavioral Health Billing
Billing regulations and payer requirements can vary significantly by state. Working with a provider that understands regional nuances can make a significant difference.
For example:
Providers offering behavioral health billing maine services must navigate specific Medicaid policies
A behavioral health billing services company florida must align with state-specific insurance regulations
Clinics seeking the best behavioral health billing services company new york benefit from expertise in high-volume urban healthcare systems
Choosing a behavioral health billing company in california ensures compliance with complex state healthcare laws
This localized knowledge helps reduce claim rejections and improves reimbursement rates.
Why “Behavioral Health Billing Services Near Me” Searches Are Increasing
Healthcare providers increasingly search for behavioral health billing services near me because proximity often implies better communication and understanding of local payer systems.
However, with advanced technology, many top providers now offer nationwide services while still maintaining expertise in regional billing practices. This allows clinics to access the best outsource behavioral health billing and coding services regardless of location.
Key Features of a High-Quality Behavioral Health Billing Solution
A reliable healthcare behavioral health billing solution should offer more than basic billing. It should integrate seamlessly with your practice operations.
Essential features include:
Real-time reporting and analytics
Electronic health record (EHR) integration
Automated claim tracking
Denial trend analysis
Custom dashboards for financial insights
These features ensure transparency and help providers make informed decisions.
Common Mistakes in Behavioral Health Billing
Even experienced providers can make billing mistakes that impact revenue.
Some common issues include:
Incorrect use of time-based CPT codes
Missing or incomplete documentation
Failure to verify insurance eligibility
Ignoring payer-specific billing rules
Delayed claim submissions
Working with a professional behavioral health billing company helps eliminate these errors and improves overall efficiency.
In-House vs Outsourced Behavioral Health Billing
Many providers struggle to decide whether to manage billing internally or outsource it.
In-House Billing:
Greater control over operations
Higher staffing and training costs
Increased risk of errors
Outsourced Billing:
Access to industry experts
Reduced operational costs
Scalable and efficient processes
This is why outsourcing behavioral health billing and coding has become the preferred model for growing practices.
How a Top Behavioral Health Billing Agency Improves Revenue
A well-established behavioral health billing services company focuses on optimizing every stage of the revenue cycle.
They achieve this by:
Reducing claim denials through accurate coding
Speeding up reimbursements with clean claims
Identifying revenue leakage points
Improving patient billing processes
Choosing the best behavioral health billing company new york or any other region ensures your practice remains financially stable and compliant.
The Future of Behavioral Health Billing in the USA
The behavioral health sector is rapidly evolving, with increased demand for mental health services across the country.
Future trends include:
Greater use of automation and AI in billing
Increased focus on value-based care models
Stricter compliance requirements
Integration of telehealth billing processes
To stay competitive, providers must adopt advanced behavioral health billing solutions and partner with experienced professionals.
Why Partnering with the Right Billing Company Matters
A professional behavioral health billing company is more than just a service provider—it’s a growth partner. By improving accuracy, reducing denials, and ensuring compliance, they directly impact your bottom line.
Companies like 247 Medical Billing Services support healthcare providers with end-to-end solutions including medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services. These integrated offerings help practices streamline operations and focus on delivering high-quality patient care.
Conclusion
Behavioral health billing is complex, time-consuming, and critical to the financial health of any practice. Partnering with a professional behavioral health billing company ensures accuracy, compliance, and improved revenue performance.
Whether you are a small clinic or a large healthcare organization, outsourcing behavioral health billing can transform your operations. From reducing administrative burden to maximizing reimbursements, the right partner plays a crucial role in your success.
Investing in expert billing services is not just about managing claims—it’s about building a sustainable and scalable healthcare practice.
FAQs
What is a professional behavioral health billing company?
A professional behavioral health billing company specializes in managing billing, coding, and revenue cycle processes for mental health and substance abuse treatment providers.
Why should I outsource behavioral health billing services?
Outsourcing improves accuracy, reduces costs, and ensures compliance while allowing providers to focus on patient care.
How do behavioral health billing services differ from general medical billing?
They involve time-based coding, therapy sessions, and stricter documentation requirements, making them more complex.
Can a billing company help reduce claim denials?
Yes, experienced providers use accurate coding, proper documentation, and payer-specific guidelines to minimize denials.
Is it better to choose a local billing company?
While local expertise can help, many nationwide providers offer specialized services tailored to different states.
What should I look for in the best behavioral health billing services company?
Look for experience, transparency, advanced technology, compliance expertise, and strong denial management processes.
How does outsourcing behavioral health billing and coding improve revenue?
It ensures faster claim processing, fewer errors, and better reimbursement rates, leading to improved cash flow.