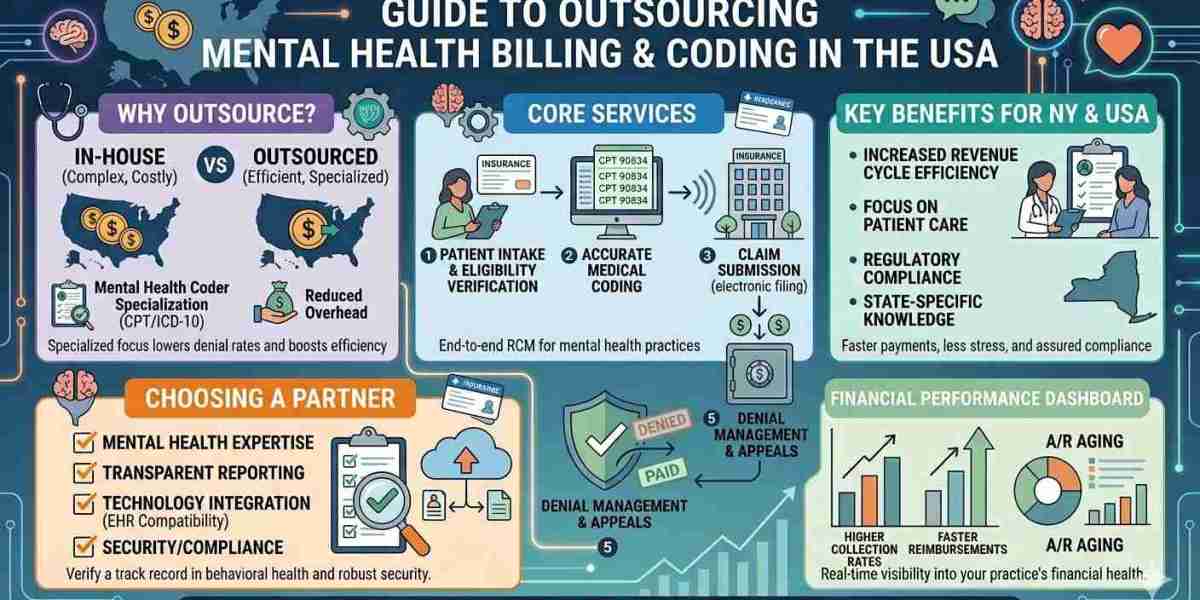
Behavioral health practices across South Carolina are facing increasing administrative pressure, stricter payer rules, and rising denial rates. Finding the best behavioral health billing company south carolina is no longer just an operational choice—it directly impacts revenue, compliance, and patient care quality. Whether you run a private therapy clinic, a community mental health center, or a multi-location practice, the right billing partner can transform your financial performance.
This guide explores what makes a billing company truly effective, how to evaluate your options, and why outsourcing has become the preferred strategy for behavioral health providers.
Why Behavioral Health Billing Requires Specialized Expertise
Behavioral health billing is significantly more complex than general medical billing. It involves unique coding structures, session-based billing, strict documentation requirements, and varying payer policies.
Common challenges include:
Frequent claim denials due to incorrect CPT or ICD coding
Complex pre-authorization and medical necessity requirements
Compliance with evolving mental health regulations
Delayed reimbursements affecting cash flow
Coordination with Medicaid, Medicare, and commercial payers
Practices often struggle to maintain in-house teams that can keep up with these complexities. This is why many providers are turning toward outsourcing behavioral health billing services to experienced partners.
Key Benefits of Choosing the Right Billing Partner
Selecting the best behavioral health billing company south carolina offers several measurable benefits:
Improved claim acceptance rates through accurate coding
Faster reimbursement cycles with reduced AR days
Lower operational costs compared to in-house teams
Better compliance with state and federal regulations
More time for providers to focus on patient care
Many providers who previously relied on internal teams have transitioned to outsourcing behavioral health billing ohio or outsourcing behavioral health billing services connecticut to benchmark efficiency and scalability across different regions.
What Defines the Best Behavioral Health Billing Company
Not all billing companies deliver the same level of service. The best partners stand out based on specific capabilities:
Industry-Specific Experience
A specialized billing company understands behavioral health nuances such as therapy session limits, telehealth billing, and substance use disorder claims.
Advanced Technology Integration
Top companies use billing software that integrates seamlessly with EHR systems, ensuring smooth data flow and minimal errors.
Denial Management Expertise
Efficient denial tracking and resubmission processes are critical. Practices benefit from partners who proactively identify patterns and prevent recurring issues.
Transparent Reporting
Detailed financial reports help providers track performance, revenue trends, and payer behavior.
Compliance and Security
HIPAA compliance and secure data handling are non-negotiable for behavioral health providers.
Providers often compare services across regions, including outsourcing behavioral health billing services delaware and outsourcing behavioral health billing services florida, to identify companies with consistent performance standards.
Why South Carolina Providers Are Moving Toward Outsourcing
Healthcare providers in South Carolina are increasingly adopting outsourcing models due to:
Shortage of skilled billing professionals locally
Rising administrative costs
Increased regulatory complexity
Need for scalable solutions as practices grow
Outsourcing behavioral health billing texas and outsourcing behavioral health billing virginia have shown how regional outsourcing strategies can significantly improve revenue cycle efficiency.
Similarly, many organizations are exploring outsourcing behavioral health medical billing services provider in florida to leverage experienced teams with multi-state expertise.
Comparing Billing Services Across States
To understand what makes a company the best, it helps to compare services offered across different regions:
A professional behavioral health billing company new hampshire may focus on smaller practices with personalized services
Behavioral health billing services rhode island often emphasize compliance and documentation accuracy
Behavioral health billing services connecticut are known for strong payer relationships
Behavioral health billing services north carolina focus on scalability for growing clinics
Looking at a professional behavioral health billing company connecticut or a professional behavioral health billing company rhode island can provide insights into best practices that South Carolina providers can adopt.
Key Services You Should Expect
When evaluating a billing partner, ensure they offer comprehensive services such as:
Insurance verification and eligibility checks
Accurate CPT and ICD coding
Claims submission and tracking
Payment posting and reconciliation
Denial management and appeals
Accounts receivable follow-up
Financial reporting and analytics
Providers comparing behavioral health billing columbus or behavioral health billing columbus ohio often highlight the importance of end-to-end service coverage rather than partial support.
How Location-Specific Expertise Impacts Performance
Billing requirements can vary by state due to differences in Medicaid policies, payer rules, and compliance regulations.
For example:
Behavioral health billing company california may focus heavily on telehealth billing compliance
Behavioral health billing services in california often handle high patient volumes with complex payer mixes
Behavioral health billing company georgia may specialize in Medicaid-heavy claims
Behavioral health medical billing utah may emphasize rural healthcare billing challenges
Understanding these differences helps South Carolina providers choose a company with the right experience and adaptability.
Community Behavioral Health Billing Needs
Community health organizations have unique billing challenges, including grant funding, sliding fee scales, and high patient volumes.
Many providers look into outsourcing community behavioral health billing ohio or working with a community behavioral health billing services company delaware to manage these complexities efficiently.
These organizations require billing partners who can handle:
Multi-payer environments
Government program compliance
Detailed reporting for funding audits
Signs You Need a Better Billing Company
If your practice is experiencing any of the following issues, it may be time to switch providers:
Increasing claim denial rates
Delayed reimbursements
Lack of financial transparency
Frequent coding errors
Overburdened administrative staff
Exploring options like a top behavioral health billing company virginia or reviewing behavioral health billing ohio services can help identify better-performing partners.
How to Choose the Best Behavioral Health Billing Company South Carolina
When making your final decision, consider these steps:
Evaluate the company’s experience in behavioral health billing
Request performance metrics such as claim acceptance rates
Check client testimonials and case studies
Assess technology and integration capabilities
Ensure compliance with HIPAA and state regulations
Ask about scalability for future growth
A well-informed decision ensures long-term financial stability and operational efficiency.
The Role of Technology in Modern Billing
Modern billing companies leverage advanced tools to improve accuracy and efficiency:
AI-driven coding assistance
Automated claim scrubbing
Real-time eligibility verification
Data analytics for revenue optimization
These technologies reduce manual errors and accelerate reimbursement cycles, making them essential for any high-performing billing partner.
Future Trends in Behavioral Health Billing
The behavioral health billing landscape is evolving rapidly. Key trends include:
Increased adoption of telehealth billing
Value-based care reimbursement models
Integration of AI in revenue cycle management
Greater emphasis on compliance and data security
Providers who align with forward-thinking billing companies will be better positioned for long-term success.
Conclusion
Choosing the best behavioral health billing company south carolina is a strategic decision that directly affects your practice’s financial health and operational efficiency. With increasing complexities in behavioral health billing, outsourcing has become the most reliable way to ensure accuracy, compliance, and consistent revenue growth.
A trusted partner like 247 Medical Billing Services can support your practice with comprehensive solutions including medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services. By aligning with an experienced billing company, providers can focus on delivering quality patient care while maintaining a strong financial foundation.
FAQs
What makes a behavioral health billing company the best in South Carolina?
The best company offers specialized expertise, high claim acceptance rates, transparent reporting, and strong compliance practices tailored to behavioral health services.
Is outsourcing better than in-house billing for behavioral health practices?
Yes, outsourcing often reduces costs, improves accuracy, and ensures faster reimbursements compared to maintaining an in-house billing team.
How do billing companies reduce claim denials?
They use accurate coding, claim scrubbing tools, and proactive denial management strategies to identify and fix errors before submission.
Can a billing company handle multi-state behavioral health practices?
Experienced billing companies can manage multi-state operations by adapting to different payer rules and compliance requirements.
What services should a behavioral health billing company provide?
Comprehensive services include coding, claims submission, AR follow-up, denial management, reporting, and credentialing support.
How long does it take to see results after outsourcing billing?
Most practices begin to see improvements in claim approvals and cash flow within the first 60 to 90 days.