Mental health practices across the United States are growing rapidly, but managing finances remains one of the biggest challenges. From complex coding requirements to strict payer rules, billing for mental health therapists requires precision, compliance, and consistency. Many therapists struggle to balance patient care with administrative responsibilities, making efficient billing systems essential for long-term success.
This guide provides a clear, practical breakdown of how mental health billing works, the common challenges therapists face, and how to optimize your revenue cycle without compromising care quality.
Key Highlights of Mental Health Billing
- Accurate documentation ensures faster claim approvals and fewer denials
- Proper coding directly impacts reimbursement rates
- Insurance verification reduces claim rejection risks
- Outsourcing can improve efficiency and reduce operational costs
- Compliance with Medicare and private payers is critical
Understanding Billing for Mental Health Therapists
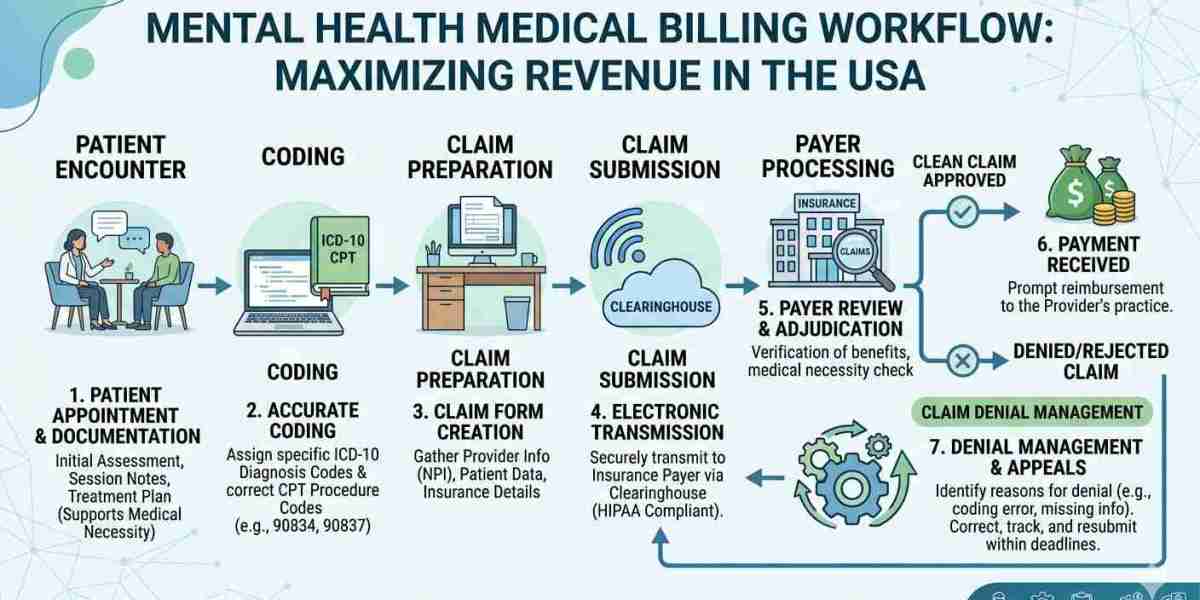
Billing for mental health therapists involves submitting claims for services such as psychotherapy, counseling, psychiatric evaluations, and medication management. Unlike general medical billing, mental health billing requires a deeper understanding of session-based coding, time-based CPT codes, and payer-specific requirements.
Whether you run a solo practice or a large clinic, billing for mental health providers must be handled with accuracy to avoid revenue loss. The process includes patient intake, insurance verification, coding, claim submission, payment posting, and denial management.
Why Mental Health Billing is More Complex Than General Medical Billing
Mental health billing differs from traditional medical billing in several ways:
Time-Based Coding
Therapy sessions are billed based on duration, which makes precise documentation essential. Even small discrepancies can lead to claim denials.
Authorization Requirements
Many insurance providers require pre-authorization for mental health services, especially for ongoing therapy sessions.
Strict Documentation Standards
Detailed clinical notes are necessary to justify treatment and ensure compliance with payer guidelines.
Frequent Policy Changes
Rules around billing medicare for mental health services and private insurers change often, requiring continuous updates.
Because of these complexities, many practices turn to mental health billing services to streamline operations.
Essential Components of Mental Health Billing
1. Insurance Verification
Before providing services, verifying patient eligibility helps reduce claim denials and ensures accurate reimbursement.
2. Coding and Billing for Mental Health Services
Correct use of CPT and ICD codes is the backbone of successful billing. Coding errors can delay payments or result in rejected claims.
3. Claim Submission
Timely submission of clean claims improves cash flow and minimizes delays.
4. Payment Posting and Reconciliation
Tracking payments ensures that providers receive the correct reimbursement for services rendered.
5. Denial Management
Analyzing and correcting denied claims is critical for recovering lost revenue.
Common Challenges in Mental Health Billing
Many therapists face recurring issues when handling billing for mental health services:
- High claim denial rates due to coding errors
- Delays in reimbursement from insurance companies
- Difficulty managing administrative workload
- Lack of expertise in billing medicare for mental health services
- Compliance risks due to improper documentation
These challenges often push providers toward outsourcing mental health billing and coding to experienced professionals.
Benefits of Outsourcing Mental Health Billing
Outsourcing has become a popular solution for therapists looking to improve efficiency and revenue.
Reduced Administrative Burden
By outsourcing mental health billing, therapists can focus more on patient care rather than paperwork.
Improved Revenue Cycle
Professional billing companies for mental health ensure faster claim processing and fewer denials.
Access to Experts
A mental health billing services company brings specialized knowledge in coding, compliance, and payer requirements.
Cost Efficiency
Working with a cheap outsource mental health billing company can be more affordable than maintaining an in-house team.
Scalability
Outsourced billing for mental health allows practices to grow without increasing administrative overhead.
Choosing the Right Mental Health Billing Partner
Selecting the right partner is critical for success. Here are some factors to consider:
Experience in Mental Health Billing
Look for mental health billing specialist companies that understand therapy-specific billing nuances.
Comprehensive Services
A top mental health billing company should offer end-to-end solutions, including credentialing, coding, and denial management.
Technology Integration
Modern mental health billing solutions should integrate with your EHR system for seamless operations.
Transparency and Reporting
The best mental health billing company provides clear reports and regular updates on performance.
Compliance Expertise
Ensure the provider follows HIPAA regulations and payer-specific guidelines.
In-House vs Outsourced Billing: What’s Better?
In-House Billing
Pros:
- Full control over processes
- Direct communication with staff
Cons:
- Higher operational costs
- Requires continuous training
- Increased risk of errors
Outsourced Billing
Pros:
- Access to experts
- Reduced administrative workload
- Better claim acceptance rates
Cons:
- Less direct control
- Requires choosing a reliable partner
For most practices, outsourcing mental health billing offers better efficiency and profitability.
Best Practices for Efficient Mental Health Billing
To improve your billing process, follow these proven strategies:
Maintain Accurate Documentation
Clear and detailed notes support claims and reduce denials.
Stay Updated on Coding Changes
Regular updates in coding and billing for mental health services ensure compliance.
Verify Insurance Before Every Session
This prevents unexpected claim rejections.
Track Key Performance Metrics
Monitor claim acceptance rates, denial rates, and reimbursement timelines.
Use Professional Billing Services
Partnering with billing services for mental health clinics improves overall efficiency.
Role of Technology in Mental Health Billing
Modern technology plays a vital role in optimizing billing processes. Advanced software helps automate claim submission, track payments, and identify errors before submission.
Mental health billing and credentialing services often include integrated platforms that streamline operations and reduce manual work. These systems also improve transparency and reporting, helping providers make informed decisions.
How Mental Health Billing Impacts Revenue Growth
Efficient billing directly influences a practice’s financial health. Poor billing practices can lead to revenue leakage, delayed payments, and compliance risks.
By implementing structured mental health medical billing processes or partnering with a reliable mental health billing company, practices can:
- Increase claim approval rates
- Reduce administrative costs
- Improve cash flow
- Enhance patient satisfaction
When Should You Consider Outsourcing?
You should consider outsourcing mental health billing if:
- Your claim denial rate is increasing
- Administrative workload is overwhelming
- Revenue cycle performance is declining
- You lack expertise in billing for mental health therapists
- Compliance requirements are becoming difficult to manage
Partnering with the best outsource mental health billing and coding services can help resolve these challenges efficiently.
Conclusion
Billing for mental health therapists is a complex but critical aspect of running a successful practice in the United States. From accurate coding to compliance and denial management, every step plays a role in ensuring consistent revenue.
Whether you choose to manage billing in-house or work with a mental health billing services company, the key is to maintain accuracy, stay compliant, and continuously optimize your processes. For many providers, outsourcing mental health billing proves to be the most effective way to improve efficiency and focus on delivering quality care.
For practices looking to streamline operations, 247 Medical Billing Services offers comprehensive support including medical billing services, medical coding services, medical billing and coding services, revenue cycle management services, and credentialing services, helping providers achieve sustainable growth without administrative stress.
Frequently Asked Questions
What is billing for mental health therapists?
Billing for mental health therapists refers to the process of submitting and managing insurance claims for therapy and psychiatric services to ensure proper reimbursement.
Why is mental health billing complicated?
It involves time-based coding, strict documentation requirements, and varying insurance policies, making it more complex than general medical billing.
Is outsourcing mental health billing a good option?
Yes, outsourcing mental health billing can reduce administrative workload, improve accuracy, and increase revenue.
What services do mental health billing companies provide?
They handle insurance verification, coding, claim submission, payment posting, denial management, and compliance.
How can I improve my mental health billing process?
Focus on accurate documentation, proper coding, regular insurance verification, and consider working with experienced billing services for mental health.
Do mental health billing companies handle Medicare claims?
Yes, most experienced providers manage billing medicare for mental health services along with private insurance claims.
What should I look for in a billing partner?
Choose a provider with experience, transparency, advanced technology, and expertise in behavioral and mental health billing services.