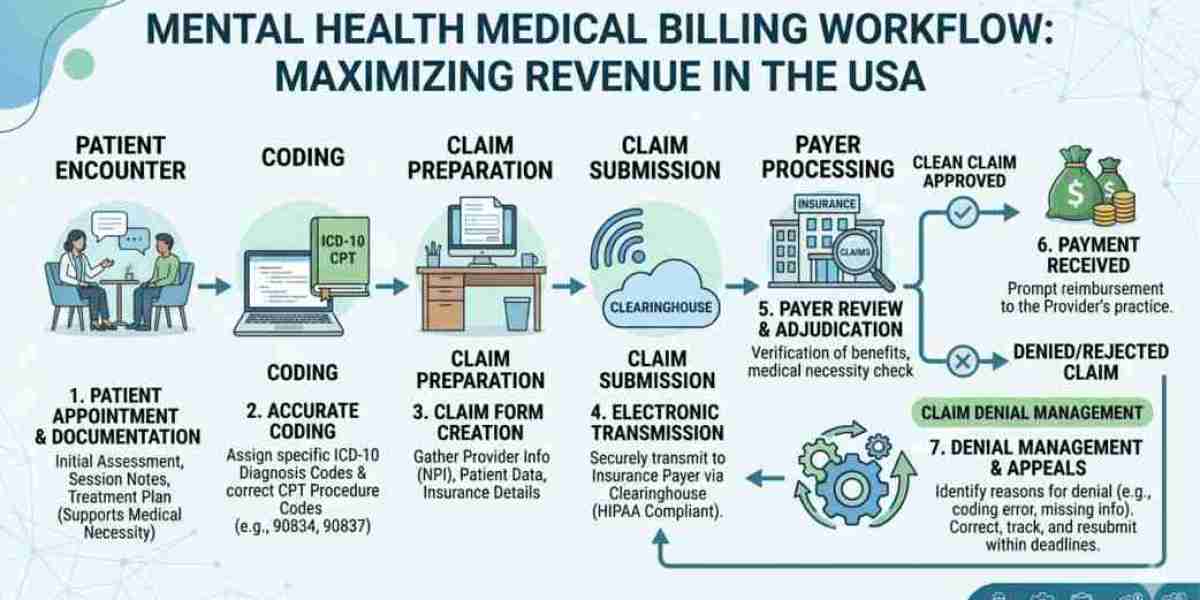
Mental health practices across the United States are growing rapidly, but so are the complexities of getting paid. From navigating insurance rules to maintaining compliance with ever-changing regulations, billing for mental health providers has become one of the most critical—and challenging—parts of running a successful practice.
Whether you are a solo therapist, group practice owner, psychiatrist, or behavioral health clinic, understanding how to manage billing effectively can directly impact your revenue, patient satisfaction, and operational efficiency.
This guide breaks down everything you need to know in a clear, practical way so you can optimize your billing workflow without feeling overwhelmed.
Why Billing for Mental Health Providers Is Different
Unlike general medical billing, mental health billing involves unique challenges:
Session-based billing instead of procedure-heavy coding
Frequent use of time-based CPT codes
Pre-authorization requirements for many services
Strict documentation standards
High claim rejection rates due to minor errors
Because of these factors, many practices rely on mental health insurance billing services or a dedicated mental health billing specialist to handle claims accurately and efficiently.
Key Components of Mental Health Billing
To build a strong billing system, you need to understand the core components involved:
1. Patient Eligibility Verification
Before providing services, verifying insurance coverage is essential. This step confirms:
Coverage for therapy or psychiatric services
Copay, coinsurance, and deductible details
Authorization requirements
Skipping this step often leads to claim denials and delayed payments.
2. Accurate Coding
Mental health billing depends heavily on proper coding:
CPT codes for therapy sessions (e.g., 90834, 90837)
ICD-10 codes for diagnoses
Modifiers when required
Working with a mental health billing and coding company helps ensure accuracy and compliance.
3. Claim Submission
Clean claims are submitted electronically to insurance companies. Errors at this stage can result in:
Rejections
Delays
Revenue loss
Many providers adopt a mental health medical billing solution to automate this process.
4. Payment Posting and Reconciliation
Once claims are processed:
Payments are posted
Adjustments are recorded
Denials are tracked
5. Denial Management
Denied claims must be analyzed, corrected, and resubmitted quickly. This is where a mental health billing consultant can add significant value.
Common Challenges in Mental Health Billing
Even experienced providers face obstacles such as:
Frequent Claim Denials
Errors in coding, missing documentation, or incorrect patient details can lead to denials.
Changing Insurance Policies
Insurance guidelines for behavioral health change frequently, making it difficult to stay updated.
Time-Consuming Administrative Work
Billing tasks take time away from patient care.
Compliance Risks
Incorrect billing practices can lead to audits and penalties.
Because of these challenges, many practices choose to outsource mental health billing services to professionals who specialize in behavioral health.
Benefits of Outsourced Mental Health Billing
Outsourcing is becoming the preferred choice for many providers. Here’s why:
Improved Revenue Cycle
Professional teams ensure faster claim processing and reduced denials.
Access to Expertise
A mental health billing agency or mental health billing companies bring specialized knowledge that general billing teams may lack.
Cost Efficiency
Hiring and training in-house staff can be expensive. Outsourced mental health billing reduces overhead costs.
Focus on Patient Care
Providers can dedicate more time to patients instead of administrative tasks.
Compliance and Accuracy
A professional mental health billing company stays updated with regulations and payer requirements.
Choosing the Right Mental Health Billing Partner
Selecting the right billing partner is crucial for long-term success. Consider the following:
Experience in Behavioral Health
Look for a mental health billing provider with proven experience in mental health and psychiatry billing.
Technology and Tools
A reliable mental health medical billing services outsourcing partner should use advanced billing software for:
Claim tracking
Reporting
Analytics
Transparency
Choose a mental health billing services agency that provides clear reporting and communication.
Customization
Your billing needs may vary. The best outsource mental health billing and coding company will tailor services to your practice.
End-to-End Services
Top outsource mental health billing company options offer complete solutions including:
Credentialing
Coding
AR follow-up
Denial management
In-House vs Outsourced Billing: What Works Best?
In-House Billing
Pros:
Full control
Immediate access to billing staff
Cons:
High costs
Training requirements
Risk of errors
Outsourced Billing
Pros:
Expertise and accuracy
Reduced administrative burden
Better revenue performance
Cons:
Less direct control
For most growing practices, outsourced mental health billing offers a scalable and efficient solution.
Best Practices for Effective Mental Health Billing
To optimize billing performance, follow these best practices:
Maintain Accurate Documentation
Clear and detailed notes are essential for claim approval.
Verify Insurance Before Every Visit
Policies can change frequently, so always confirm eligibility.
Use Correct Codes
Incorrect coding is one of the top reasons for denials.
Track Key Metrics
Monitor:
Claim acceptance rate
Days in AR
Denial rate
Stay Updated on Regulations
Compliance is critical in mental health billing.
Partner with Experts
Working with billing services for mental health therapists ensures better outcomes.
The Role of Technology in Mental Health Billing
Modern billing systems play a huge role in improving efficiency. A strong mental health medical billing solution can:
Automate claim submission
Reduce human errors
Provide real-time reporting
Improve revenue tracking
Technology combined with expert support creates a powerful billing ecosystem.
How Billing Impacts Patient Experience
Billing isn’t just about revenue—it also affects patient satisfaction.
Transparent and accurate billing:
Builds trust
Reduces confusion
Improves payment collection
A well-managed system, whether in-house or through a mental health billing agency, ensures a smoother experience for patients.
Why Many Providers Are Switching to Outsourcing
The demand for mental health services is increasing, and providers need scalable solutions. That’s why many practices are moving toward:
Mental health insurance billing handled by experts
Outsourced mental health billing for efficiency
Partnerships with top mental health billing companies
This shift allows providers to grow without being limited by administrative challenges.
How 247 Medical Billing Services Supports Mental Health Providers
For practices looking to streamline operations and improve revenue, partnering with an experienced team makes a significant difference.
247 Medical Billing Services offers comprehensive support including medical billing services, medical coding services, and medical billing and coding services tailored for behavioral health practices. Their expertise extends to revenue cycle management services and credentialing services, helping providers maintain compliance, reduce denials, and optimize cash flow.
By combining industry expertise with advanced technology, they provide a complete solution for billing services for mental health providers.
Conclusion
Billing for mental health providers is more than just submitting claims—it’s a critical part of maintaining a sustainable and successful practice. With increasing complexities in insurance policies and compliance requirements, relying solely on traditional methods can limit growth.
Whether you choose to build an in-house team or partner with a professional mental health billing consultant, the goal remains the same: accurate billing, faster reimbursements, and improved patient experience.
Investing in the right systems and support today can transform your revenue cycle and allow you to focus on what truly matters—delivering quality mental health care.
FAQs
What is billing for mental health providers?
It is the process of submitting and managing insurance claims for therapy, psychiatry, and behavioral health services to ensure providers are reimbursed accurately.
Why is mental health billing complex?
It involves time-based codes, strict documentation requirements, and varying insurance policies, making it more detailed than general medical billing.
Should I outsource mental health billing?
If managing billing internally is time-consuming or leading to errors, outsourced mental health billing can improve efficiency and revenue.
What does a mental health billing specialist do?
They handle coding, claim submission, denial management, and compliance specifically for mental health services.
How do I choose the best mental health billing agency?
Look for experience, transparency, advanced technology, and a proven track record in behavioral health billing.
What are the benefits of mental health medical billing services?
They reduce administrative workload, improve claim accuracy, and help maximize reimbursements.
Can billing errors affect patient experience?
Yes, inaccurate billing can cause confusion and dissatisfaction, making efficient billing systems essential.