Mental health practices across the USA are growing rapidly, but so are the complexities of billing, coding, and insurance compliance. For therapists, psychologists, and behavioral health clinics, managing finances is no longer just about sending claims—it’s about accuracy, compliance, and consistent cash flow. That’s where a mental health billing specialist becomes essential.
Whether you're a solo therapist or managing a multi-provider clinic, understanding how specialized billing support works can significantly impact your bottom line and reduce administrative stress.
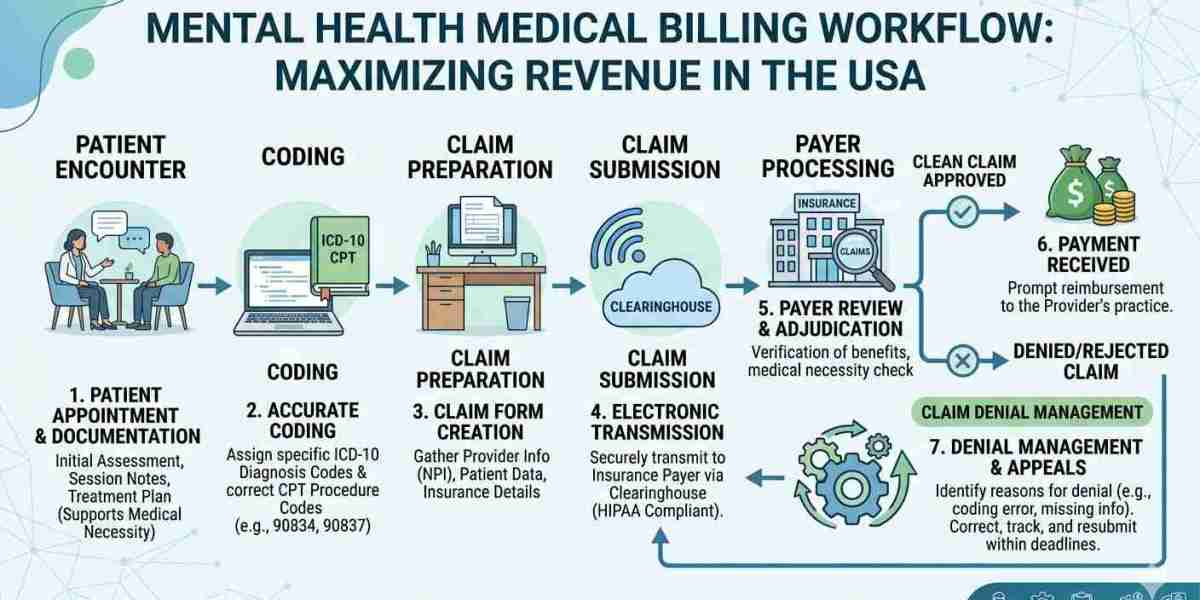
The Growing Complexity of Mental Health Billing
Mental health billing isn’t as straightforward as general medical billing. It involves:
- Frequent coding updates for psychotherapy sessions
- Strict documentation requirements
- Pre-authorizations and insurance verification
- Variations in payer policies across states
A small error—like incorrect CPT codes or missing modifiers—can delay payments or lead to denials. This is why many providers are now turning to mental health insurance billing services to ensure accuracy and efficiency.
What Does a Mental Health Billing Specialist Do?
A mental health billing specialist focuses exclusively on behavioral health services. Their expertise goes beyond basic claim submission.
Key Responsibilities
- Accurate CPT and ICD-10 coding for therapy sessions
- Insurance verification and eligibility checks
- Claim submission and tracking
- Denial management and appeals
- Payment posting and reconciliation
Unlike general billing staff, specialists understand nuances like time-based therapy codes, telehealth billing, and payer-specific mental health rules.
Why Providers Choose to Outsource Mental Health Billing Services
Managing billing in-house can quickly become overwhelming. Hiring, training, and retaining skilled staff requires time and resources. This is why many clinics choose to outsource mental health billing services.
Benefits of Outsourcing
- Reduced administrative burden
- Faster claim processing
- Improved claim acceptance rates
- Lower operational costs
- Access to industry experts
Outsourcing also allows providers to focus on patient care instead of paperwork.
Choosing the Best Mental Health Billing Agency
Not all billing partners are created equal. Selecting the best mental health billing agency requires careful evaluation.
What to Look For
- Experience in behavioral health billing
- Transparent pricing models
- Strong denial management process
- HIPAA compliance
- Real-time reporting and analytics
A reliable mental health billing services agency acts as an extension of your practice, ensuring your revenue cycle runs smoothly.
How Mental Health Medical Billing Services Improve Revenue
A well-managed billing system directly impacts your financial health. Professional mental health medical billing services help optimize every stage of the revenue cycle.
Key Improvements
- Reduced claim rejections
- Faster reimbursements
- Improved cash flow
- Better compliance with insurance regulations
When combined with a structured mental health medical billing solution, practices can scale without worrying about revenue leakage.
Tailored Billing Services for Mental Health Therapists
Therapists often face unique billing challenges—especially those in private practice. Specialized billing services for mental health therapists address these issues directly.
Common Challenges Solved
- Session-based billing errors
- Insurance credentialing delays
- Managing multiple payers
- Tracking patient balances
With the right support, therapists can focus more on patient outcomes rather than financial management.
The Role of a Mental Health Billing and Coding Company
A dedicated mental health billing and coding company ensures that both billing and coding processes are aligned. This reduces errors and increases efficiency.
Why Coding Accuracy Matters
Incorrect coding can result in:
- Claim denials
- Compliance risks
- Revenue loss
This is why integrating medical coding services with billing processes is critical for long-term success.
Outsourced Mental Health Billing: A Scalable Solution
As practices grow, so do billing demands. Outsourced mental health billing provides scalability without increasing internal workload.
Ideal for:
- Growing group practices
- Telehealth providers
- Multi-location clinics
Working with a top outsource mental health billing company ensures that your billing operations expand seamlessly alongside your practice.
Mental Health Billing Companies vs In-House Teams
Many providers debate whether to build an internal team or partner with external mental health billing companies.
In-House Billing
- Higher staffing costs
- Ongoing training required
- Risk of errors due to limited expertise
Outsourced Billing
- Access to trained professionals
- Lower overhead costs
- Better claim success rates
For most practices, partnering with a mental health billing agency offers better ROI and fewer headaches.
The Bigger Picture: Revenue Cycle Management in Mental Health
Billing is just one part of the financial ecosystem. Comprehensive revenue cycle management services cover everything from patient registration to final payment.
Core Components
- Patient eligibility verification
- Charge capture
- Claim submission
- Payment posting
- Denial management
When integrated properly, revenue cycle management ensures consistent income and financial stability.
Why Credentialing Services Matter
Before billing even begins, providers must be enrolled with insurance companies. This is where credentialing services come into play.
Importance of Credentialing
- Enables insurance reimbursements
- Builds provider credibility
- Prevents claim rejections
Delays in credentialing can result in lost revenue, making it a crucial step in the billing process.
Integrating Medical Billing and Coding Services
For optimal efficiency, practices should combine medical billing services and medical billing and coding services under one system.
Benefits of Integration
- Fewer errors
- Faster claim processing
- Better compliance
- Improved financial tracking
This integrated approach ensures that both clinical and financial data align accurately.
Real-World Example: A Growing Therapy Practice
Consider a mid-sized therapy clinic in Texas that struggled with delayed payments and high denial rates. After switching to mental health medical billing services outsourcing, they experienced:
- 35% reduction in claim denials
- 25% faster reimbursement cycles
- Significant reduction in administrative workload
This shift allowed therapists to focus entirely on patient care while experts handled the financial side.
Why Practices Trust 247 Medical Billing Services
Many healthcare providers are now turning to experienced partners like 247 medical billing services to streamline their operations. By combining:
- medical billing services
- medical coding services
- medical billing and coding services
- revenue cycle management services
- credentialing services
they offer a comprehensive solution tailored to mental health providers. This kind of integrated support helps practices maintain compliance, reduce errors, and improve overall financial performance without added stress.
Conclusion: The Future of Mental Health Billing in the USA
The demand for mental health services continues to rise, but so does the complexity of billing. Relying on a skilled mental health billing specialist is no longer optional—it’s a necessity for sustainable growth.
Whether you choose in-house support or decide to outsource mental health billing services, the goal remains the same: accurate billing, faster payments, and a healthier revenue cycle.
By partnering with the right experts and leveraging comprehensive solutions, mental health providers can focus on what truly matters—delivering quality care to their patients.
FAQs
1. What does a mental health billing specialist do?
A mental health billing specialist manages claim submission, coding, insurance verification, and denial handling specifically for behavioral health services.
2. Is it better to outsource mental health billing services?
Yes, outsourcing often reduces costs, improves claim accuracy, and allows providers to focus more on patient care rather than administrative tasks.
3. How do mental health billing services improve revenue?
They minimize errors, reduce claim denials, and speed up reimbursements, leading to consistent cash flow.
4. What should I look for in a mental health billing agency?
Look for experience in behavioral health, transparency, compliance standards, and strong reporting capabilities.
5. Why are credentialing services important?
Credentialing ensures providers are approved by insurance companies, enabling them to receive reimbursements without delays.
6. Can small therapy practices benefit from billing services?
Absolutely. Even solo therapists can benefit from professional billing services by saving time and improving revenue efficiency.